Where is COVID-19 headed next? North.
There are many factors affecting the level of COVID-19 affliction across cities around the globe, but as we map the spread of the virus it appears that temperature and humidity play determining roles that are worth digging into.
The impact of temperature and humidity on the survival rate of viruses has been known since the 1960s [1, 2, 3]. Put simply, viruses like it best when it’s dry and chilly [4, 5]. Research shows that the sweet spot for SARS COV 2, if it acts like other viruses, could be between 5-11℃ with an average specific humidity of 5g/kg [6, 7, 8, 9,10,11].
Within buildings, research on this topic amassed over the course of several years, has helped to inform the development of the RESET Standard and underpins the requirements for continuous monitoring of temperature and humidity. Whereas the relationships between human health and particulate matter, chemical emissions (VOCs) and CO2 are now well documented, temperature & humidity are typically only peripherally acknowledged because of their association with human comfort.
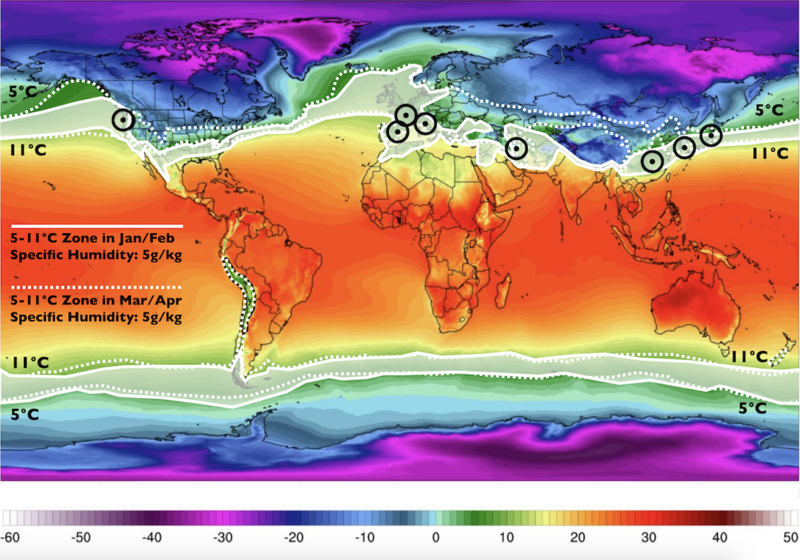
To illustrate the critical relationship between temperature, humidity and human health, have a look at the diagram below: it documents areas most heavily afflicted by COVID-19 in February. All of them fall within the same temperature zones and have similar humidity profiles. All of them were similarly chilly and dry at the time.
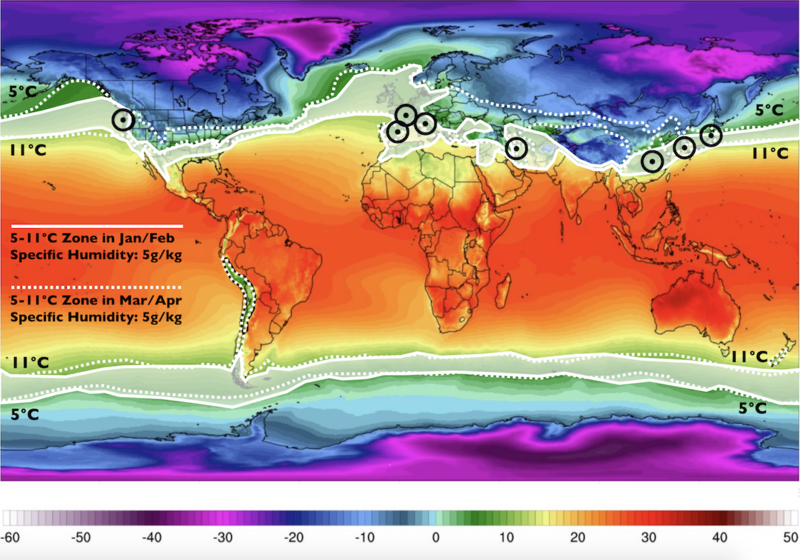
World temperature map November 2018-March 2019. Color gradient indicates 2-meter temperatures in ℃. Black circles represent countries with significant community transmission (> 10 deaths as of March 10, 2020). Base Image from Climate Reanalyzer https://ClimateReanalyzer.org, Climate Change Institute, University of Maine, USA. Graphic adapted from “Temperature, humidity, and latitude analysis to predict potential spread and seasonality for COVID-19”[6].
What’s particularly notable regarding this pattern is how outdoor conditions appear to have a dramatic effect on a virus that has been largely associated with indoor transmission, where people are in close contact to one another.
However, contact transmission may only be one of the factors enabling viral transmission to flourish - the right environmental conditions play a catalyzing role. If proximity to one another was sufficient the flu season would be flat: in other words, there would be no seasonality at all; we would be infected year-round. After all, most of us spend as much time indoors with our colleagues irrespective of whether or not its summer or winter.
The distinction with the cold temperature season is that we heat our buildings. And when we do, the air becomes drier. And as the air becomes drier, viruses survive longer, and the rate of transmission goes up. This is likely buffered somewhat by the inverse effect that heat has on viruses [12,13].
But here’s the kicker: the indoor conditions described above exist in every cold climate, which means theoretically every region north of the 11℃ temperature line should have been equally affected. However, that’s not the case: the areas of greatest affliction seem to lie within the narrow 5-11℃ temperature band (and specific humidity of 5g/kg) that wraps the planet. In February that included Hubei (Wuhan), Iran, Northern Italy, Spain and the Seattle area.
This suggests that either most viral transmission is happening outdoors or, that we’re doing something to bring the perfect outdoor conditions inside, like perhaps over-ventilating our buildings. Spoiler alert: it’s likely to be the latter.
We know that SARS COV 2 does not survive well in ambient air and is almost immediately killed by exposure to ultraviolet light (UV irradiation) [14,15]. This means the virus is unlikely to be found freely floating around in outdoor air. We also know that transmission is mostly due to direct contact, both person-to-person and person-to-surface [16, 17, 18, 19]. As per above, this suggests that there is something we’re doing to bring those ideal outdoor conditions inside, accentuating the impact of direct contact and most likely foster airborne spread as well. More research on this topic is needed.
For now, the most important insight provided by this map is that of suggesting where SARS COV 2 will be striking next. As we head into spring, the answer seems clear: North (in both hemispheres).
When these maps were first made in late February & early March, the predicted areas of affliction for the weeks to come based on temperature and humidity were, New York, Vancouver, London, Manchester, Berlin, Prague, Hamburg, Warsaw, Glascow, Kiev, St. Louis and Beijing.
Meanwhile, cities like Bangkok which should have been hit hard, weren’t. At a balmy average temperature of 28°C and specific humidity of 16.5 g/kg, it seems the virus couldn’t get a strong hold.
These trends are important to consider given the current shortage of global resources available for treating COVID-19. Perhaps more than any other data, temperature and humidity patterns suggest where we need to be focusing the bulk of our efforts.
However, before everyone in Canada, Northern U.S., UK., Northern Europe and Central Asia starts to panic, several important notes need to be added.
- Based on temperature and humidity patterns within the areas most affected, theory is that the virus seems to need a period of stability of about 1 month to spread.
- As a result, it seems that areas likely to be most at risk are those that transition slowly through Spring.
- Although temperature is easier for most people to relate too, humidity plays an equally important (if not larger) role in the survival of viruses. For this however, we will need to shift our focus from relative humidity to specific humidity (more on this below).
- Cities and regions would be wise to study their historic temperature and specific humidity records as we change seasons.
- And not to ignore the Southern Hemisphere; New Zealand, Australia, South Africa, Argentina and Chile are all at risk from June through September.
Over the past few weeks, the real-estate industry has been in a reactionary state of panic and shock as office towers and retail centers around the world have emptied out. Buildings are seen as being a key part of the problem.
Meanwhile, the industry has been scrambling to understand whether buildings can be part of the solution. The answer is yes. As you can most likely guess, it boils down to the proper management of temperature, humidity, filtration and sterilization. It’s not rocket science, but it does need to be done properly. We’ll be sharing more in our next post.
Meanwhile, if you're interested in learning more about how building owners have been leveraging RESET in their crisis and recovery strategies for COVID-19, and how we can help you, don't hesitate to reach out.
Footnote: Specific vs. Relative Humidity, what’s the difference?
If you were one of the smart ones reading and thinking, “Seattle is chilly, but it isn’t dry.” Read on.
Imagine a roomful of air. At low temperature, the air struggles to hold much water. For the sake of this exercise, let’s say that a 5°C the air in the room is only able to hold a maximum of 5 grams before it starts to rain indoors. Now, let’s say the air was actually holding 4 grams of water. Relative humidity in the room would be 4/5 = 80% (Very humid).
Now imagine the same room heated to 30°C. At that temperature, the air can hold up to 20 grams of water. However, if the air still holds the same amount of water as before (4 grams), the relative humidity is now 4/20 = 20% (Very dry).
Meanwhile, specific humidity would be the same for both. Specific humidity measures the actual amount of water held in the air. In both cases above, 4 grams within the same quantity of air.
Although Seattle seemed relatively humid (pun intended) in February, with an average RH = 82%, the average specific humidity was a perfect 5 g/kg.
Credits
Having studied pure & applied sciences but not being a scientist, I have a soft spot for researchers who have the ability to take data and make it both relevant and easy to understand. At the top of that list is Mohammad M. Sajadi MD, Parham Habibzadeh MD, Augustin Vintzileos PhD, Shervin Shokouhi MD, Fernando Miralles-Wilhelm PhD and Anthony Amoroso MD, who’s original publication can be found here.
References
- Schaffer FL, Soergel ME, Straube DC (1976) Survival of airborne influenza virus: effects of propagating host, relative humidity, and composition of spray fluids. Arch Virol 51: 263–273. View Article. Google Scholar.
- Harper GJ (1961) Airborne micro-organisms: survival tests with four viruses. J Hyg (Lond) 59: 479–486. View Article. Google Scholar.
- Hemmes JH, Winkler KC, Kool SM (1960) Virus survival as a seasonal factor in influenza and poliomyelitis. Nature 4748: 430–431. View Article. Google Scholar.
- Lowen AC, Mubareka S, Steel J, Palese P. Influenza virus transmission is dependent on relative humidity and temperature. PLoS Pathog. 2007;3:e151. PMC free Article. PubMed. Google Scholar.
- Steel J, Palese P, Lowen AC. Transmission of a 2009 pandemic influenza virus shows a sensitivity to temperature and humidity similar to that of an H3N2 seasonal strain. J Virol. 2011;85:1400–1402. PMC free Article. PubMed. Google Scholar.
- Sajadi, Mohammad M. and Habibzadeh, Parham and Vintzileos, Augustin and Shokouhi, Shervin and Miralles-Wilhelm, Fernando and Amoroso, Anthony, Temperature, Humidity and Latitude Analysis to Predict Potential Spread and Seasonality for COVID-19 (March 5, 2020). View Article SSRN. View Article.
- Tamerius JD, Shaman J, Alonso WJ, Bloom-Feshbach K, Uejio CK, Comrie A, Viboud C. 2013. Environmental predictors of seasonal influenza epidemics across temperate and tropical climates. PLo.
- Shaman J, Pitzer VE, Viboud C, Grenfell BT, Lipsitch M. 2010. Absolute humidity and the seasonal onset of influenza in the continental United States. PLoS Biol. 8:e1000316. View Article.
- Shoji M, Katayama K, Sano K. 2011. Absolute humidity as a deterministic factor affecting seasonal influenza epidemics in Japan. Toho.
- Lowen AC, Steel J. Roles of Humidity and Temperature in Shaping Influenza Seasonality, Department of Microbiology and Immunology, Emory University School of Medicine, Atlanta, Georgia, USA. View Article.
- Anice C Lowen , Samira Mubareka, John Steel, Peter Palese. Influenza Virus Transmission Is Dependent on Relative Humidity and Temperature. Published: October 19, 2007. View Article.
- Duan SM, Zhao XS, Wen RF, Huang JJ, Pi GH, Zhang SX, Han J, Bi SL, Ruan L, Dong XP; SARS Research Team. Stability of SARS coronavirus in human specimens and environment and its sensitivity to heating and UV irradiation. View Article.
- Chan KH, Peiris JS, Lam SY, Poon LL, Yuen KY, Seto WH. The Effects of Temperature and Relative Humidity on the Viability of the SARS Coronavirus. View Article.
- Duan SM, Zhao XS, Wen RF, Huang JJ, Pi GH, Zhang SX, Han J, Bi SL, Ruan L, Dong XP; SARS Research Team. Stability of SARS coronavirus in human specimens and environment and its sensitivity to heating and UV irradiation. View Article.
- Jensen MM. Inactivation of airborne viruses by ultraviolet irradiation. Appl Microbiol. 1964;12:418–420. PMC Free Article. PubMed. Google Scholar.
- Q. Li, X. Guan, P. Wu, X. Wang, L. Zhou, Y. Tong, et al. Early transmission dynamics in Wuhan, China, of novel coronavirus-infected pneumonia N Engl J Med (2020 Jan 29), 10.1056/NEJMoa2001316. [Epub ahead of print]. Google Scholar.
- D. Wang, B. Hu, C. Hu, F. Zhu, X. Liu, J. Zhang, et al.Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China JAMA (2020 Feb 7), 10.1001/jama.2020.1585. [Epub ahead of print]. Google Scholar.
- D. Chang, M. Lin, L. Wei, L. Xie, G. Zhu, C.S. Dela Cruz, et al.Epidemiologic and clinical characteristics of novel coronavirus infections involving 13 patients outside Wuhan, China JAMA (2020 Feb 7), 10.1001/jama.2020.1623. [Epub ahead of print]. Google Scholar.
- W.G. Carlos, C.S. Dela Cruz, B. Cao, S. Pasnick, S. JamilNovel Wuhan (2019-nCoV) coronavirus Am J Respir Crit Care Med, 201 (2020), pp. P7-P8, 10.1164/rccm.2014P7. Cross Reference. Google Scholar.
